TEE for Left Atrial Appendage Closure
FoCUS How-to, Apical 4 Chamber
POCUS for Surgery

Welcome to our excellent lecture series! All our content is provided free of charge. We feel strongly about the value of perioperative ultrasound and know that motivated students already have enough roadblocks. BUT!! We need to justify the upkeep of this site to our institution. If you value this content please let me know, just a quick note from each of you (to joshua.zimmerman@hsc.utah.edu) will help!
There is a lot of confusing language and acronyms in the arena of ultrasound. What we’re basically talking about here is ultrasound provided at the point of care, at the patient’s bedside. The “bedside” could be the preop clinic, the OR, the wards, the ER, the ICU, or wherever you interact with your patients.
When we use the acronym PoCUS we mean point-of-care ultrasound. Unless you’re a cardiologist or radiologist this is what you’re likely to be doing (and if you are, you’ll be doing PoCUS sometimes too.) PoCUS can include cardiac ultrasound, vascular for access or DVT, lung, abdominal, musculoskeletal, ultrasound guided regional anesthesia, ocular, and more. It would technically also include perioperative TEE. Whatever type of ultrasound or where it’s performed, the exam is done by the physician rather than a sonographer and is interpreted in real time. When we refer to FoCUS we mean focused cardiovascular ultrasound, which is a subset of PoCUS because it’s performed at the point of care. I’ll make the distinction between FoCUS and limited TTE in the lectures below.
Why Focused Cardiac Ultrasound: A Case-Based Discussion (30 min)
- If you wonder why cardiac ultrasound is for you, take a look at this talk. If you’re already convinced you can watch it because it’s a fun talk but you could also move onto the vast sea of ‘How-to’ below.
What exactly is ”FoCUS”? (30 min)
- An introduction to the concept of FoCUS as described by the American Society of Echocardiography (and interpreted by our echo group.) Before you embark on your ultrasound training it is important for us to be on the same page regarding not only the immense value of these techniques but also their limitations.
Cardiac Anatomy for the New Echocardiographer (20 min)
- A brief review of anatomy to refresh your memory before beginning to scan. Remember that the image is not the thing, and we’re always trying to construct a mental picture of our patient’s actual anatomy from the images we create.
HeartWorks How-to (10 min)
- An introduction to the use of the excellent, valuable HeartWorks simulator. I would encourage you all to make use of simulation frequently during your ultrasound training. It might be useful to listen to this lecture while you’re actually working with the simulator. Obviously not everyone will have access to one of these, sorry!
Basic Concepts of Ultrasound (22 min)
- Don’t be scared, this isn’t your college physics class reprised. You don’t have to be able to calculate a Doppler shift to start using ultrasound in your practice, I promise! You do need a basic understanding of how an ultrasound image is formed, how to adjust basic image settings, and what common artifacts look like. That’s what Dr. Decou will review here.
FoCUS How-To (90 min)
- It’s hard to spend too much time with the basics, and these are absolutely the basics. What do you do when you put the probe on the patient? Watch these talks now, then come back to them as you continue to develop your skills.
FoCUS How-To Article
- I’m not sure, this may count as a shameless plug. This is a link to my recent article in Anesthesia and Analgesia that describes the performance of FoCUS. There is a link in the article to another how-to video and the graphics and clips in the article should serve as good examples.
Global Left Heart Evaluation (30 min)
- Assessment of the structure and global function of the left ventricle with Dr. Bledsoe. The goal here is not to distinguish between an ejection fraction of 34% vs 36%! We want to know if our patients’ LV function is not too bad, not so good, or terrible.
Global Assessment of the Right Ventricle (30 min)
- Similar concepts apply to Dr. Bledsoe’s discussion of global right ventricular function. We’d like to know if our patient’s problem (clinical evidence of heart failure, hemodynamic instability, etc) could be related to global dysfunction of the right ventricle.
Basic LV Regional Wall Motion Evaluation (2o min)
- Identification of subtle regional wall motion abnormalities is challenging even for very experienced echocardiographers. What you’re trying to identify is large areas of hypokinesis that could explain hypotension, or perhaps areas of scar that suggest old myocardial infarctions. These are less subtle. In this talk Dr. Curtis will review concepts of normal and abnormal myocardial wall motion and sequelae of infarction.
Basic Valvular Assessment (80 min)
- In this series of three lectures, we’ll review the normal anatomy of the aortic, mitral, and tricuspid valves as well as discuss findings of significant valvular stenosis and regurgitation.
FoCUS to the Rescue! (120 min)
- In this series of lectures, I’ll review the application of FoCUS in the assessment of the hemodynamically unstable patient. This topic is a ton of fun, but there’s a lot to cover so I’ve broken the 200-some slides into more bite-sized portions.
Point of Care Lung Ultrasound – Part 1, Intro and PTX (30 min)
- Pneumothorax is one of the easiest critical questions to address with bedside ultrasound, and this lecture will get you started.
Point of Care Lung Ultrasound – Part 2, Fluid (20 min)
- This is slightly more advanced lung ultrasound, get ready. This talk reviews the evaluation of pleural effusion and pulmonary edema.
Point of Care DVT Ultrasound (30 min)
- Do you take care of patients who are hypercoagulable, pregnant, have cancer, are immobile, have trauma, undergo major surgery? Of course you do! Do you ever have unstable patients where you’re considering the possibility of DVT with PE? Yes, yes. Can you perform limited ultrasound to identify DVT? You will soon!
Point of Care Gastric Ultrasound (30 min)
- Take a curvilinear probe, put it over your stomach, watch that thing trying to digest your breakfast, and then try to tell me this isn’t awesome! (Coming soon…)
**If you’re attending one of our FoCUS workshops, you can stop with the above**
TTE for the Expert Perioperative Echocardiographer
- The FoCUS lectures above provide an introduction to bedside cardiac ultrasound for the physician with limited or no experience in echocardiography. These lectures are the next level, for those with experience in TEE who “only” need to add transthoracic windows to their arsenal. We’ll add some quantification of chamber size, systolic function, valvular disease, and diastolic function. Piece of cake, right?
-
Introduction and Parasternal Imaging (35 minutes)
-
Apical Imaging (35 minutes)
-
Subcostal Imaging (15 minutes)
Lung Ultrasound for Water
Another awesome dyspnea
This 65 year-old man has a history of coronary artery disease with CABG in 2004 and presents with worsening dyspnea and atypical chest pain. The findings here are awesome and subtle, what’s the diagnosis. Also, I have been tinkering with the “blog settings” to try to keep the obnoxious spam answers out, so let me know if you have trouble posting.
Need video clips
Cause of dyspnea?
This patient presents with worsening dyspnea on exertion to the point of exertional near-syncope. This image is classic for which diagnosis?
Describe the Valve
Describe this valve. A number of different versions have been made by multiple manufacturers. What are the two most common in the US? What complication is common and with which version?
What valve disease?
OK, maybe isn’t necessarily an interesting case, but the clips are cool. What are we looking at here?

Simple Case of Chest Pain
This 84 year-old woman presented to the ED with new onset of chest pain. What’s the diagnosis?
Name the Valve
This patient is scheduled for redo valve surgery. What valve is seen at 6 o’clock in this image? Describe its function.
Most Common Abnormality to Miss?
This young patient was “minding his own business” when he suffered a stab wound to the chest. He was brought to the OR emergently for cardiac tamponade when the following images were seen. What is the other abnormality identified? Why is it seen where it is?

First Day…First Case
In some ways it is hard to beat this case. Not because of the complexity of the diagnosis, but because of its classic nature. This case was from one of our recent residency graduates. It was literally the first case he was scheduled to do on his first day as an attending anesthesiologist. The patient is a 72 year-old woman scheduled to undergo a laparoscopic hernia repair. She has chronic pain which significantly limits her mobility, but she does not report symptoms of heart failure. On physical exam, she has a harsh 4/6 systolic murmur. The image below is the first one obtained…need I go on?
If that isn’t enough, look at the next 3 images and quantify the severity based on 4 criteria. Then read this article and remember that ultrasound is the stethoscope of the future!


What? More hypotension?
Great case from Dr. Gnadinger. This patient underwent TTE shortly after the onset of severe dyspnea and chest pain. The patient is light-headed and hypotensive. Look at this image first, what would this alone tell you?
Now look at this sweet clip and tell me what’s what.
Hypotension Again!
Hot off the presses! This is a real patient from the OR today and they were profoundly hypotensive. What do we see here and what does it mean?
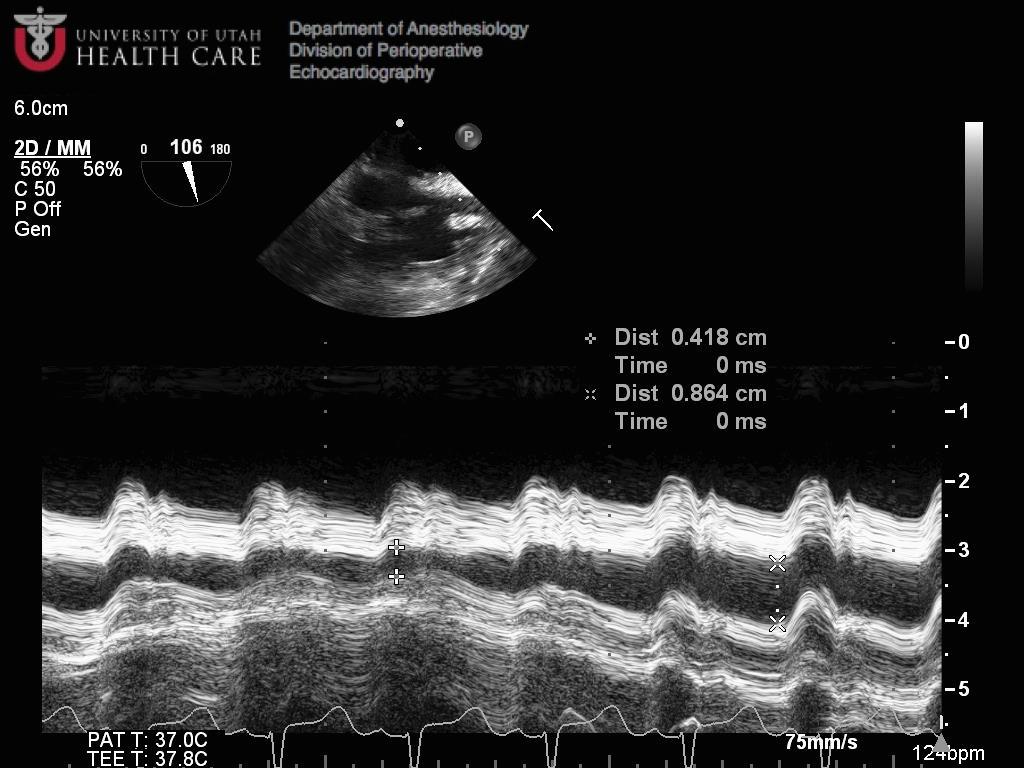
Echo Rorschach #1
What does this vegetation look like to you? (There are currently two correct answers to this echo Rorschach)
(Remember, if you can’t see the clips try using Google Chrome as your browser.)
What’s the Diastology?
Simple question. What will the mitral valve inflow show and why?
(Remember, if you can’t see the clips try using Google Chrome as your browser.)
Today’s Admission, Progressive Dyspnea
Today’s case isn’t rocket science, but it is a good one to review. This 67 year-old man is admitted to the medicine service for progressive dyspnea on exertion. He now has class III heart failure symptoms. What is going on here and how can you tell?
(Remember, if you can’t see the clips try using Google Chrome as your browser.)
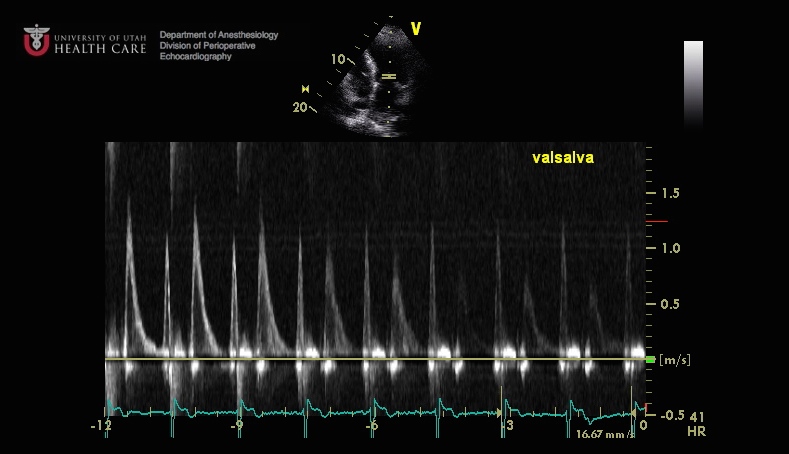
Heart Failure Exacerbation
This 58 year old man with a long history of heart murmur and Class II heart failure symptoms presents with an acute CHF exacerbation. Describe the findings in these two images. What explains the acute decompensation? What is unusual about this particular presentation.
(Remember, if you can’t see the clips try using Google Chrome as your browser.)
Intraoperative Hypotension – Why?
Why did this 39 year-old man become profoundly hypotensive after the induction of general anesthesia? What characteristics from the preoperative TTE could have predicted that? What causes these findings?
(Remember, if you don’t see the clips below try using Google Chrome as your browser.)